Poor maternity tolerated as normal
-
MRPMWoodman

- May 13, 2024
- 0
- 8 min read

Poor maternity tolerated as normal
Medical Disclaimer: You understand that any information and content, such as text, graphics, and images, found within our Website is for general educational, entertainment, and informational purposes only.
You understand that such information is not intended nor otherwise implied to be medical advice or a substitute for medical advice, diagnosis, or treatment.(Case Study or News article)

https://banzaijapan.jp – A DePRESSeD Media Ltd Website – Cospanic Entertainment Video
Poor maternity tolerated as normal
Systemic Failings Described as 'Normalised'
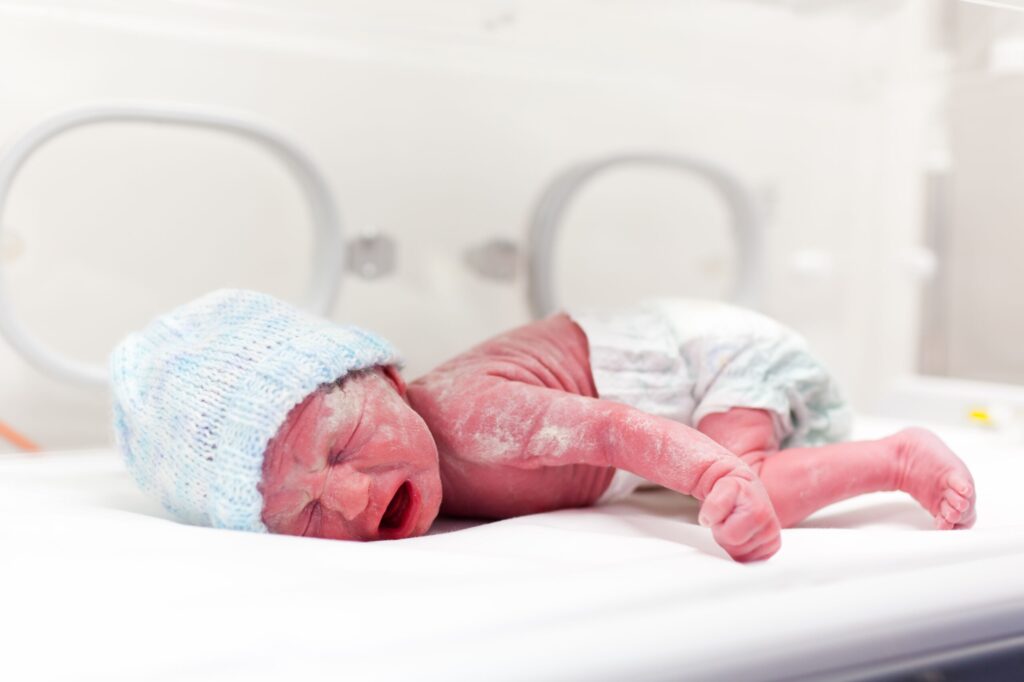
An independent review into maternity services at a major NHS trust has concluded that poor standards of care were tolerated as normal over many years. The report found repeated instances of medical negligence, particularly in the recognition and response to fetal distress during labour, which contributed to preventable baby deaths and severe brain injuries.
Investigators described a culture where substandard monitoring, delayed escalation, and inadequate senior oversight became accepted practice. Medical negligence in these areas was not challenged effectively, allowing harm to continue despite clear warning signs and national guidelines.
The review examined dozens of cases where babies suffered hypoxic-ischaemic encephalopathy or stillbirth. In multiple instances, medical negligence was identified as a direct or contributory cause — most commonly through failure to interpret abnormal CTG traces correctly or act with sufficient urgency.
Culture of Acceptance and Missed Opportunities
The report highlighted that concerning patterns of care were repeatedly identified in internal audits and incident reports, yet meaningful change was not implemented. Poor maternity care was effectively normalised within parts of the service, with staff becoming desensitised to risks that should have triggered immediate action.
Whistleblowers who raised concerns about medical negligence in fetal monitoring and timely delivery often felt dismissed or faced resistance. This defensive culture discouraged open reporting and learning, allowing medical negligence to persist and contribute to avoidable harm over an extended period.
The review team noted that junior staff and midwives sometimes hesitated to challenge decisions, while senior clinicians did not always provide the oversight required. Medical negligence became embedded in routine practice because it was not consistently confronted or corrected.
Impact on Babies and Bereaved Families
The consequences of tolerated poor maternity care were devastating. Babies who could have been born healthy suffered profound brain damage or death due to delays that amounted to medical negligence. Families were left with lifelong grief, disability support needs, and unanswered questions.
Bereaved parents described years of fighting for recognition that medical negligence had played a role in their loss. Many felt blamed or gaslighted when raising legitimate concerns about care, adding insult to the original injury caused by preventable failings.
The report confirmed what families had long suspected: medical negligence was not isolated but part of a pattern where poor standards were tolerated as normal. This normalisation directly increased the risk of harm and eroded trust in the maternity service.
Categories: Medical Negligence, Maternity Safety, Patient Safety, NHS Failings
Keywords: poor maternity tolerated, medical negligence normalised, preventable baby deaths, fetal distress failure, maternity review findings, NHS trust culture, delayed intervention negligence
Trust Leadership and Accountability
The trust’s senior leadership has accepted the review’s findings and apologised unreservedly to families affected by medical negligence. The chief executive acknowledged that poor maternity care was tolerated for too long and that the organisation must take full responsibility for allowing medical negligence to become normalised.
Significant changes have been introduced, including mandatory enhanced CTG training, 24/7 consultant presence on labour wards, revised escalation protocols, and strengthened governance to challenge substandard practice. The trust states these reforms aim to eradicate the culture that tolerated medical negligence.
However, many families and campaigners remain cautious. They argue that cultural change takes years and requires sustained leadership commitment, adequate staffing, and zero tolerance for complacency if medical negligence is to be truly eliminated from maternity services.
National Lessons from the Review
The report’s conclusion that poor maternity care was tolerated as normal has national implications. Similar patterns of delayed response to fetal distress and failure to escalate have appeared in other major maternity inquiries, suggesting systemic vulnerabilities across the NHS.
Experts call for mandatory implementation of evidence-based safety bundles, regular external audits, and protected time for senior review during labour. Preventing medical negligence requires consistent application of best practice rather than leaving it to local variation.
The review team recommended stronger whistleblower protections, regular independent oversight, and a just culture where raising concerns about medical negligence is encouraged and acted upon swiftly. These measures are seen as essential to stop poor standards being tolerated anywhere in maternity care.
Family Campaign and Ongoing Advocacy
Bereaved parents and those whose children live with disabilities caused by medical negligence have campaigned for years for this level of scrutiny. They welcomed the report’s honest assessment that poor maternity care was tolerated as normal but insist that words must now turn into sustained action.
The families continue to support each other and speak publicly about their experiences. They want every maternity unit to treat fetal distress with the urgency required so that medical negligence no longer results in preventable death or life-changing injury.
Their determination reflects a refusal to accept that medical negligence should ever be considered normal. They hope the report’s findings force genuine, lasting reform across the NHS maternity system and beyond.
Urgency for Cultural and Systemic Change
Patient safety organisations stress that normalising poor maternity care represents a profound failure of leadership and governance. Medical negligence becomes tolerated when warning signs are ignored, concerns are dismissed, and accountability is weak.
The report serves as a powerful call to break this cycle. Trusts must foster cultures where excellence is the norm, medical negligence is challenged immediately, and families receive openness and compassion when things go wrong.
Until poor maternity care is no longer tolerated as normal, the risk of preventable harm will remain. The families affected by medical negligence in this case hope their pain drives the urgent, comprehensive change needed to make every birth as safe as possible.
Categories: Medical Negligence, Maternity Safety, Patient Safety, NHS Failings
Keywords: poor maternity tolerated, medical negligence normalised, preventable baby deaths, fetal distress failure, maternity review findings, NHS trust culture, delayed intervention negligence, maternity safety reform
Medical Negligence
Medical negligence, also known as clinical negligence (particularly in the UK), occurs when a healthcare professional provides substandard care that falls below the reasonable standard expected of a competent practitioner in similar circumstances, directly causing harm or injury to a patient.To succeed in a claim, four key elements (often referred to as the “4 Ds”) must typically be proven:
- Duty of care — A doctor-patient or similar professional relationship existed, establishing that the healthcare provider owed the patient a duty to provide competent treatment.
- Breach of duty (or deviation from the standard of care) — The care provided was negligent, meaning it did not meet the accepted professional standards. This is assessed objectively, often with input from independent medical experts, rather than requiring “gold standard” treatment.
- Causation — The breach directly caused (or significantly contributed to) the patient’s injury or worsened condition. The harm must be more likely than not attributable to the substandard care.
- Damage — The patient suffered actual harm, which may include physical injury, psychological distress, financial loss, additional medical needs, or reduced quality of life.
Common examples include misdiagnosis, delayed diagnosis, surgical errors, incorrect medication, failure to obtain informed consent, or inadequate aftercare. Not every poor outcome or medical mistake constitutes negligence—only those deviating from reasonable professional standards and causing avoidable harm qualify.In the UK, claims are pursued through the civil justice system, often against the NHS or private providers, with the goal of securing compensation to address losses and support recovery. Medical negligence cases can be complex, requiring expert evidence and strict time limits for claims.
Home Page – Medical Negligence – Medical Negligence – Medical Negligence – Home Page – Home Page – Banzai Japan – Home Page – Home Page –

https://sekaigyakuten.jp – A DePRESSeD Media Ltd Website – Cospanic Entertainment Video


 English
English