‘Emily’ 44 Case Study
-
MRPMWoodman

- March 17, 2026
- 0
- 9 min read

‘Emily’ 44 Case Study
Medical Disclaimer: You understand that any information and content, such as text, graphics, and images, found within our Website is for general educational, entertainment, and informational purposes only.
You understand that such information is not intended nor otherwise implied to be medical advice or a substitute for medical advice, diagnosis, or treatment.(Case Study or News article)
1

https://sekaigyakuten.jp – A DePRESSeD Media Ltd Website – Cospanic Entertainment Video
'Emily’ 44 Case Study
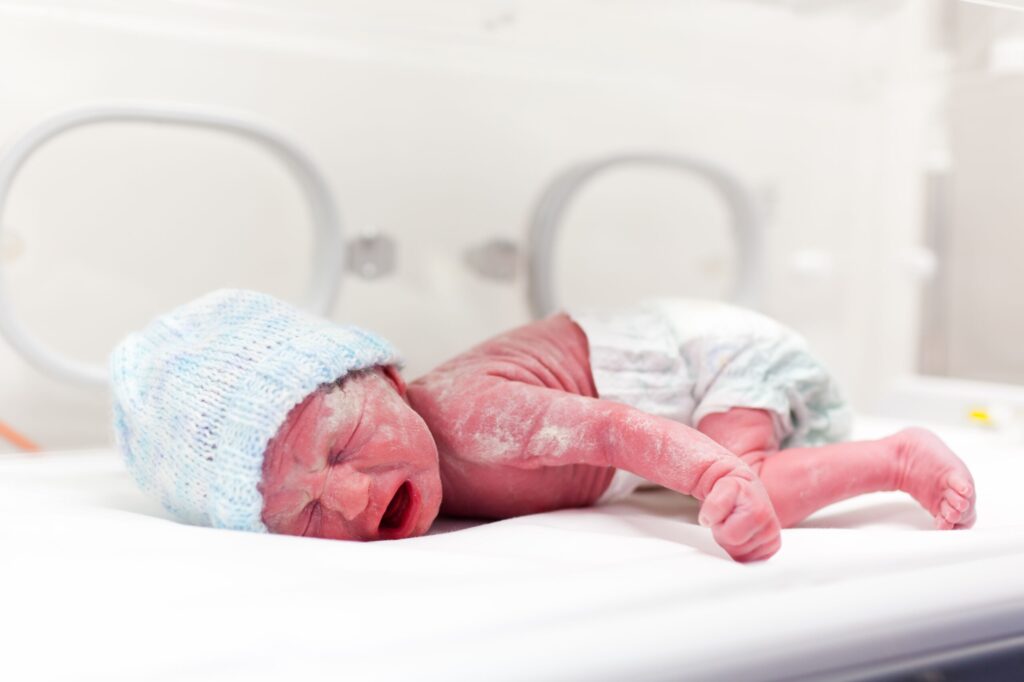
Emily’s Early Pregnancy Symptoms and Initial GP Visit
Emily, aged 44, had a history of one previous Caesarean section. When she discovered she was pregnant again she quickly booked an early scan due to spotting and mild lower abdominal pain. At her first private ultrasound appointment the sonographer noted an intrauterine gestational sac but could not clearly identify a fetal pole or heartbeat at that very early stage. She was advised to return in one week for repeat scanning.
During the following days Emily’s pain increased significantly and she began experiencing heavier vaginal bleeding. She attended her GP who recorded the symptoms but reassured her that this was likely a threatened miscarriage and arranged a hospital scan for the following week. Medical negligence began at this point: given Emily’s previous Caesarean scar and the combination of pain plus bleeding, urgent referral for specialist assessment to exclude Caesarean scar ectopic pregnancy should have been made immediately.
Emily continued to deteriorate over the next few days. The pain became severe and constant, and bleeding increased. Despite multiple contacts with both her GP and the early pregnancy unit, no same-day or next-day hospital assessment was arranged. Medical negligence in failing to recognise the high-risk features of a potential scar ectopic pregnancy allowed the condition to progress undetected and untreated.
Rupture and Emergency Life-Saving Surgery
Five days after her GP visit Emily collapsed at home with sudden, excruciating abdominal pain and heavy bleeding. She was rushed to hospital by ambulance where emergency ultrasound confirmed a ruptured Caesarean scar ectopic pregnancy with massive intra-abdominal haemorrhage. She underwent immediate laparotomy, required transfusion of multiple units of blood and had to have a hysterectomy to control life-threatening bleeding.
Medical negligence in the preceding weeks meant the ectopic pregnancy was not diagnosed or managed before rupture occurred. Had timely transvaginal ultrasound and specialist review taken place when red-flag symptoms were reported, the scar ectopic could have been identified early and treated conservatively or with planned surgery, preserving Emily’s uterus and future fertility.
As a direct result of the delay caused by medical negligence Emily is now permanently infertile, has undergone major abdominal surgery, suffered significant blood loss and faces long-term psychological trauma. The physical scarring and loss of fertility have had a profound impact on her emotional wellbeing and family planning hopes.
Categories: Medical Negligence, Ectopic Pregnancy, Delayed Diagnosis, Gynaecology Claims
Keywords: Caesarean scar ectopic negligence, medical negligence delayed diagnosis, ruptured ectopic pregnancy, preventable hysterectomy, infertility claim, early pregnancy unit failure, GP referral delay
Claim Pursued and Trust’s Admission of Liability
Emily instructed specialist medical negligence solicitors to investigate the care provided by her GP and the early pregnancy unit. Independent expert evidence from consultant gynaecologists and radiologists confirmed that medical negligence had occurred: persistent pain and bleeding in a woman with a previous Caesarean scar required urgent specialist ultrasound and referral — not repeated reassurance and delayed scanning.
The relevant NHS bodies eventually admitted full liability for medical negligence. The experts agreed that timely diagnosis of the scar ectopic pregnancy would almost certainly have allowed conservative management (methotrexate) or planned surgical removal with preservation of the uterus. The repeated failures to investigate amounted to medical negligence that directly caused the rupture, emergency hysterectomy and permanent infertility.
A substantial settlement was agreed to compensate Emily for pain and suffering, loss of fertility, psychological injury, loss of amenity, future private fertility treatment options (where possible), and the emotional impact of the preventable hysterectomy caused by medical negligence. The award provides financial security to help Emily rebuild her life after the life-altering consequences of delayed diagnosis.
Long-Term Physical and Emotional Consequences
Emily now lives with permanent infertility following the hysterectomy necessitated by medical negligence. She experiences ongoing pelvic pain from surgical scarring, early surgical menopause symptoms (hot flushes, bone density loss, mood changes) requiring hormone replacement therapy, and significant psychological trauma including depression, anxiety and grief over the loss of future fertility and family expansion.
The settlement funds private psychological counselling, hormone therapy, bone health monitoring, pain management, and support for lifestyle adjustments after medical negligence. While the compensation addresses practical and financial needs, Emily emphasises that no amount can restore her fertility or remove the emotional scars left by the preventable rupture and emergency surgery.
Emily has chosen to share her experience publicly to raise awareness of Caesarean scar ectopic pregnancy and the red-flag symptoms (pain and bleeding in early pregnancy after previous Caesarean). She hopes other women receive urgent specialist assessment so medical negligence does not lead to similar preventable loss of fertility or life-threatening complications.
Lessons from the Preventable Harm
The case demonstrates that Caesarean scar ectopic pregnancy is a rare but increasingly recognised condition that requires high clinical suspicion in women with previous Caesarean sections who present with early pregnancy pain and bleeding. Medical negligence occurs far too often when these symptoms are attributed to miscarriage or ectopic in a normal location without urgent specialist ultrasound.
National guidelines recommend early transvaginal ultrasound and senior gynaecology review for any woman with a prior Caesarean scar who develops pain or bleeding in early pregnancy. Medical negligence can be prevented through better awareness, lower threshold for specialist referral and rapid access to diagnostic imaging in early pregnancy units and primary care.
Patient safety organisations continue to campaign for improved training on scar ectopic recognition and mandatory referral pathways. Medical negligence in failing to diagnose and manage this condition promptly can lead to rupture, massive haemorrhage, emergency hysterectomy and permanent infertility — all potentially avoidable with vigilant care.
Support and Advice for Women Affected
If you or a loved one has suffered infertility, hysterectomy or other serious harm due to suspected delayed diagnosis of Caesarean scar ectopic pregnancy or other early pregnancy complications caused by medical negligence, early specialist legal advice is essential. Time limits apply (usually three years from awareness of harm caused by medical negligence), but acting promptly preserves evidence and allows access to support services.
Specialist medical negligence solicitors assess cases on a No-Win-No-Fee basis after initial review. They instruct leading gynaecologists, radiologists and fertility specialists to prove medical negligence and secure maximum compensation for physical, psychological and financial losses after preventable injury or loss of fertility.
Emily’s story serves as a powerful reminder that pain and bleeding in early pregnancy after previous Caesarean must be treated as a potential scar ectopic until proven otherwise. Medical negligence in failing to investigate urgently can have catastrophic, irreversible consequences. Prompt specialist assessment remains the key to preventing avoidable harm and preserving fertility.
Categories: Medical Negligence, Gynaecology Claims, Delayed Diagnosis, Infertility
Keywords: Caesarean scar ectopic negligence, medical negligence delayed diagnosis, ruptured ectopic pregnancy, preventable hysterectomy, infertility claim, early pregnancy unit failure, GP referral delay
Medical Negligence
Medical negligence, also known as clinical negligence (particularly in the UK), occurs when a healthcare professional provides substandard care that falls below the reasonable standard expected of a competent practitioner in similar circumstances, directly causing harm or injury to a patient.To succeed in a claim, four key elements (often referred to as the “4 Ds”) must typically be proven:
- Duty of care — A doctor-patient or similar professional relationship existed, establishing that the healthcare provider owed the patient a duty to provide competent treatment.
- Breach of duty (or deviation from the standard of care) — The care provided was negligent, meaning it did not meet the accepted professional standards. This is assessed objectively, often with input from independent medical experts, rather than requiring “gold standard” treatment.
- Causation — The breach directly caused (or significantly contributed to) the patient’s injury or worsened condition. The harm must be more likely than not attributable to the substandard care.
- Damage — The patient suffered actual harm, which may include physical injury, psychological distress, financial loss, additional medical needs, or reduced quality of life.
Common examples include misdiagnosis, delayed diagnosis, surgical errors, incorrect medication, failure to obtain informed consent, or inadequate aftercare. Not every poor outcome or medical mistake constitutes negligence—only those deviating from reasonable professional standards and causing avoidable harm qualify.In the UK, claims are pursued through the civil justice system, often against the NHS or private providers, with the goal of securing compensation to address losses and support recovery. Medical negligence cases can be complex, requiring expert evidence and strict time limits for claims.
Home Page – Medical Negligence – Medical Negligence – Medical Negligence – Home Page – Home Page – Banzai Japan – Home Page – Home Page –

https://banzaijapan.jp – A DePRESSeD Media Ltd Website – Cospanic Entertainment Video
- 'Emily’ 44 Case Study


 English
English