Lucy 30 Case Study
-
MRPMWoodman

- March 17, 2026
- 0
- 8 min read

Lucy 30 Case Study
Medical Disclaimer: You understand that any information and content, such as text, graphics, and images, found within our Website is for general educational, entertainment, and informational purposes only.
You understand that such information is not intended nor otherwise implied to be medical advice or a substitute for medical advice, diagnosis, or treatment.(Case Study or News article)
2

https://banzaijapan.jp – A DePRESSeD Media Ltd Website – Cospanic Entertainment Video
Lucy, 30 Case Study
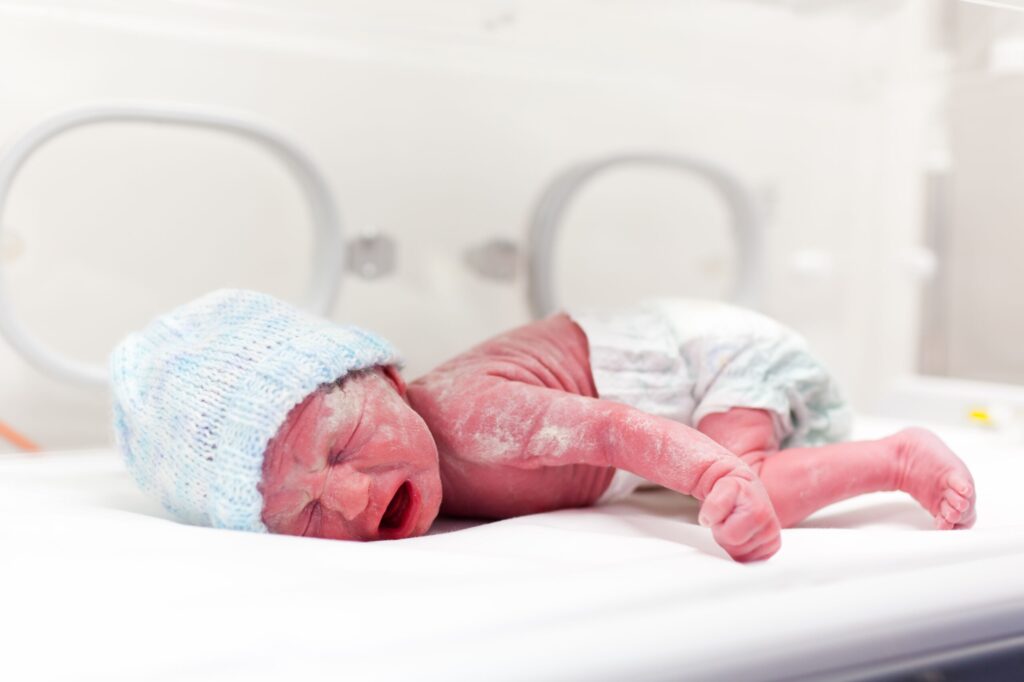
Lucy's Pregnancy and Routine Monitoring
Lucy, aged 30 and pregnant with her first child, received antenatal care at a hospital trust in the north of England. She attended all scheduled appointments and expressed normal concerns for a primigravida. Routine growth scans and monitoring were carried out, but concerns about reduced fetal movements in the third trimester were not escalated appropriately.
In the weeks leading up to the stillbirth Lucy repeatedly reported decreased fetal movements to midwives and doctors. Despite these clear warning signs — a recognised red flag for fetal compromise — medical negligence occurred when staff failed to arrange urgent review, additional monitoring or delivery. Instead she was reassured on multiple occasions and sent home with basic advice to continue kick counting.
National guidelines require immediate investigation (CTG, ultrasound assessment of liquor volume and fetal wellbeing) when reduced movements are reported, especially in the third trimester. Medical negligence in failing to follow these protocols allowed the fetus to remain in a compromised state without intervention, directly contributing to the stillbirth.
Final Appointment and Preventable Stillbirth
At her final antenatal appointment Lucy again raised concerns about significantly reduced movements over the previous 48 hours. A brief handheld Doppler was used to confirm a fetal heart rate, but no CTG monitoring, growth scan or liquor assessment was performed. Medical negligence occurred when the clinician did not recognise the urgency of the reported symptom change and discharged Lucy with follow-up in a week.
Later that evening Lucy felt no further movements. She attended the maternity unit where no fetal heart was detected on auscultation or CTG. An ultrasound confirmed intrauterine fetal death. The stillbirth was later attributed to placental insufficiency and cord compression that had been developing over days or weeks. Medical negligence in failing to investigate reduced movements earlier meant the opportunity for timely delivery was lost.
Post-mortem examination confirmed the baby was well-grown but showed signs of chronic hypoxia. Expert evidence obtained during the clinical negligence claim concluded that induction or Caesarean delivery at any of the earlier appointments when reduced movements were reported would almost certainly have resulted in a live birth.
Categories: Medical Negligence, Stillbirth, Maternity Safety, Fetal Monitoring Failure
Keywords: stillbirth medical negligence, reduced fetal movements failure, maternity negligence claim, preventable stillbirth, CTG monitoring negligence, placental insufficiency delay, NHS maternity failings
Trust Admits Liability After Expert Evidence
Lucy instructed specialist medical negligence solicitors to investigate the care provided during her pregnancy. Independent experts — consultant obstetricians and fetal medicine specialists — unanimously concluded that medical negligence had occurred. The repeated failure to investigate reported reduced fetal movements with appropriate monitoring and timely delivery breached accepted standards of care.
The hospital trust admitted full liability for medical negligence before trial. Expert reports confirmed that earlier intervention at any of the appointments when Lucy raised concerns would likely have prevented the stillbirth. The trust accepted that medical negligence in antenatal monitoring and risk assessment directly caused the tragic outcome.
A substantial settlement was agreed to compensate Lucy for the profound grief and psychological injury caused by the stillbirth, bereavement damages, funeral expenses and the loss of the parent-child relationship she was denied due to medical negligence. The award also recognises the long-term emotional impact on her mental health and future family planning.
Emotional and Psychological Impact on Lucy
Lucy now lives with lifelong grief and post-traumatic stress disorder following the stillbirth caused by medical negligence. She experiences flashbacks to the moment she was told there was no heartbeat, profound guilt despite knowing the fault lay with the care provided, and anxiety about any future pregnancies.
The settlement provides funding for ongoing psychological therapy, counselling and support groups. However, Lucy emphasises that no financial award can replace the child she lost to preventable medical negligence or remove the deep sense of injustice and betrayal she feels after trusting the maternity service with her first pregnancy.
Lucy has chosen to share her story publicly to raise awareness of reduced fetal movements as a critical warning sign. She urges all pregnant women to insist on immediate investigation if movements decrease, and hopes her case drives change so medical negligence no longer results in preventable stillbirths.
Lessons from the Preventable Stillbirth
The case demonstrates that reduced fetal movements are a genuine emergency in late pregnancy. Medical negligence occurs far too often when midwives or doctors reassure patients without objective assessment (CTG, ultrasound liquor volume, growth scan). National guidelines (Royal College of Obstetricians and Gynaecologists, NHS Saving Babies’ Lives Care Bundle) require prompt investigation and consideration of delivery when movements are significantly reduced.
Lucy’s experience highlights the need for mandatory training on reduced fetal movements awareness for all maternity staff, clear patient information leaflets, and a low threshold for admission and monitoring when concerns are raised. Medical negligence can be prevented through consistent application of these evidence-based protocols.
Patient safety organisations continue to campaign for better implementation of fetal movement awareness campaigns and rapid-access pathways. Medical negligence in failing to act on reduced movements can turn a healthy pregnancy into a tragic stillbirth — a preventable outcome with proper vigilance and response.
Support and Advice for Bereaved Parents
If you have experienced a stillbirth or neonatal death and believe medical negligence may have played a role, early specialist legal advice is essential. Time limits apply (usually three years from the date of death or awareness of medical negligence), but acting promptly preserves evidence and allows access to support services.
Specialist medical negligence solicitors assess cases on a No-Win-No-Fee basis after initial review. They instruct leading obstetricians, fetal medicine specialists and pathologists to prove medical negligence and secure maximum compensation for bereavement, psychological injury and financial losses after preventable stillbirth.
Lucy’s story serves as a powerful reminder that reduced fetal movements must always be treated as a red-flag symptom. Medical negligence in failing to investigate promptly can have catastrophic consequences. Urgent CTG monitoring, ultrasound assessment and consideration of delivery remain the key to preventing avoidable stillbirths.
Categories: Medical Negligence, Stillbirth, Maternity Safety, Fetal Monitoring Failure
Keywords: stillbirth medical negligence, reduced fetal movements failure, maternity negligence claim, preventable stillbirth, CTG monitoring negligence, placental insufficiency delay, NHS maternity failings
Medical Negligence
Medical negligence, also known as clinical negligence (particularly in the UK), occurs when a healthcare professional provides substandard care that falls below the reasonable standard expected of a competent practitioner in similar circumstances, directly causing harm or injury to a patient.To succeed in a claim, four key elements (often referred to as the “4 Ds”) must typically be proven:
- Duty of care — A doctor-patient or similar professional relationship existed, establishing that the healthcare provider owed the patient a duty to provide competent treatment.
- Breach of duty (or deviation from the standard of care) — The care provided was negligent, meaning it did not meet the accepted professional standards. This is assessed objectively, often with input from independent medical experts, rather than requiring “gold standard” treatment.
- Causation — The breach directly caused (or significantly contributed to) the patient’s injury or worsened condition. The harm must be more likely than not attributable to the substandard care.
- Damage — The patient suffered actual harm, which may include physical injury, psychological distress, financial loss, additional medical needs, or reduced quality of life.
Common examples include misdiagnosis, delayed diagnosis, surgical errors, incorrect medication, failure to obtain informed consent, or inadequate aftercare. Not every poor outcome or medical mistake constitutes negligence—only those deviating from reasonable professional standards and causing avoidable harm qualify.In the UK, claims are pursued through the civil justice system, often against the NHS or private providers, with the goal of securing compensation to address losses and support recovery. Medical negligence cases can be complex, requiring expert evidence and strict time limits for claims.
Home Page – Medical Negligence – Medical Negligence – Medical Negligence – Home Page – Home Page – Banzai Japan – Home Page – Home Page –

https://sekaigyakuten.jp – A DePRESSeD Media Ltd Website – Cospanic Entertainment Video
- Lucy 30 Case Study


 English
English