‘Eleanor’ 64 Case Study
-
MRPMWoodman

- March 17, 2026
- 0
- 8 min read

‘Eleanor’ 64 Case Study
Medical Disclaimer: You understand that any information and content, such as text, graphics, and images, found within our Website is for general educational, entertainment, and informational purposes only.
You understand that such information is not intended nor otherwise implied to be medical advice or a substitute for medical advice, diagnosis, or treatment.(Case Study or News article)

https://banzaijapan.jp – A DePRESSeD Media Ltd Website – Cospanic Entertainment Video
‘Eleanor’ 64 Case Study
Eleanor’s Initial Admission and Early Warning Signs
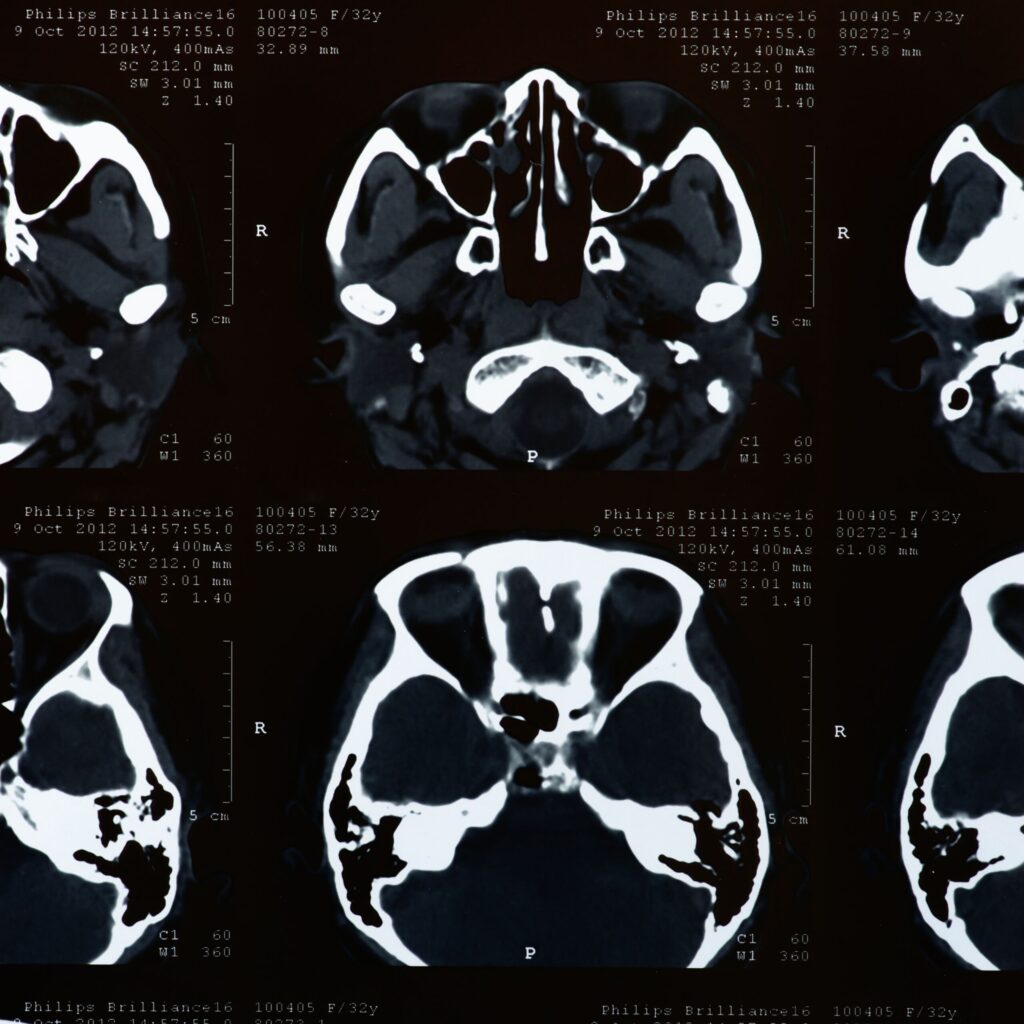
Eleanor, aged 64, was admitted to hospital with severe abdominal pain, vomiting and signs of acute illness. Initial blood tests showed significantly raised inflammatory markers and an erect chest X-ray revealed free air under the diaphragm — a classic sign of gastrointestinal perforation. Despite these clear indicators, medical negligence occurred when the surgical team did not act with appropriate urgency.
Eleanor was initially managed conservatively with intravenous fluids, antibiotics and analgesia, but her condition continued to deteriorate over the next 48 hours. She developed increasing abdominal distension, tachycardia, hypotension and rising lactate levels — all pointing to progressing peritonitis and sepsis. Medical negligence was evident in the failure to recognise the need for immediate exploratory laparotomy and source control surgery.
Over the following days Eleanor’s organ function worsened. She required escalating vasopressor support and ventilatory assistance in intensive care. The delay in surgical intervention allowed widespread peritoneal contamination and multi-organ failure to become established. Medical negligence in failing to operate promptly turned a potentially survivable perforation into a fatal cascade of sepsis and organ failure.
Progression to Death and Preventable Outcome
Despite eventual surgical exploration several days after admission, the damage from prolonged peritonitis was irreversible. Eleanor developed disseminated intravascular coagulation, acute kidney injury requiring dialysis, liver failure and refractory septic shock. She passed away in intensive care approximately one week after initial presentation. The coroner later confirmed the cause of death as multi-organ failure secondary to perforated viscus and untreated peritonitis.
Independent expert evidence obtained during the clinical negligence claim concluded that had exploratory surgery been performed within 12–24 hours of admission — as required by accepted surgical standards — Eleanor would have had a very high probability of survival with full recovery. The repeated delays amounting to medical negligence were the primary cause of her premature and avoidable death.
Eleanor’s husband and adult children pursued a fatal medical negligence claim against the hospital trust. The claim focused on the avoidable progression from a contained perforation to overwhelming sepsis due to medical negligence in surgical decision-making and escalation of care.
Categories: Medical Negligence, Fatal Medical Negligence, Sepsis & Perforation, Patient Safety
Keywords: medical negligence perforation delay, fatal sepsis negligence, delayed emergency laparotomy, preventable death hospital, gastrointestinal perforation claim, surgical negligence death, A&E medical negligence
Trust Admits Liability and Substantial Settlement
The hospital trust eventually admitted full liability for medical negligence. Expert reports from consultant general surgeons and intensivists confirmed that the repeated failure to recognise the need for urgent surgery and to escalate Eleanor’s deteriorating condition constituted gross medical negligence.
A substantial settlement was agreed on behalf of Eleanor’s estate and her dependents. The award compensated for bereavement damages, loss of dependency (financial support Eleanor would have provided), funeral expenses, psychological injury to the family and the loss of her companionship and guidance caused by medical negligence. The compensation provides essential financial security for Eleanor’s husband and children after the preventable death.
While the settlement offers practical support for the family, Eleanor’s husband emphasised that no amount can replace the wife and mother lost to medical negligence. The payout reflects the profound impact of the delay and serves as formal recognition that earlier surgical intervention should have been performed.
Long-Term Impact on Eleanor’s Family
Eleanor’s husband and adult children now live with lifelong grief following the preventable death caused by medical negligence. The sudden loss has left emotional scars, financial insecurity and the ongoing pain of knowing timely surgery could have saved her life and preserved their family unit.
The compensation helps with day-to-day living costs, memorial wishes, psychological counselling for the family and future support needs for the children. However, the family stresses that no financial award can heal the emotional void or restore the years of life and family memories lost to medical negligence.
Eleanor’s husband has chosen to share the case publicly to raise awareness of the urgency required in suspected gastrointestinal perforation. He urges medical staff to treat free air on chest X-ray and deteriorating vital signs as surgical emergencies so medical negligence does not claim other lives.
Lessons from the Preventable Death
The case demonstrates that perforated viscus is a surgical emergency. Medical negligence occurs far too often when free air under the diaphragm — a radiological sign of perforation — is not acted upon with immediate laparotomy. National guidelines require urgent surgical exploration in such cases, not conservative management or delayed review.
Eleanor’s experience highlights the need for mandatory training on recognition of perforation signs for all acute medical and surgical staff, clear escalation protocols for deteriorating patients, and a low threshold for theatre when sepsis or peritonitis is suspected. Medical negligence can be prevented through vigilant monitoring, rapid decision-making and senior involvement.
Patient safety organisations continue to campaign for better implementation of sepsis screening tools, early warning systems and rapid access to emergency surgery. Medical negligence in failing to treat perforation promptly can lead to fatal multi-organ failure — a preventable outcome with proper vigilance and response.
Support and Advice for Bereaved Families
If you have lost a loved one and believe medical negligence may have contributed to the death — such as delay in treating perforation, sepsis or other acute surgical conditions — early specialist legal advice is essential. Time limits apply (usually three years from date of death), but acting promptly preserves evidence and allows access to support services.
Specialist medical negligence solicitors assess fatal claims on a No-Win-No-Fee basis after initial review. They instruct leading surgeons, intensivists and pathologists to prove medical negligence and secure maximum compensation for bereavement, dependency losses and financial impact after preventable death.
Eleanor’s family hopes her story reminds healthcare professionals of the urgency required in suspected perforation. Medical negligence in delaying surgical intervention can have fatal consequences. Prompt recognition, resuscitation and theatre access remain the key to preventing avoidable deaths.
Categories: Medical Negligence, Fatal Medical Negligence, Sepsis & Perforation, Patient Safety
Keywords: medical negligence perforation delay, fatal sepsis negligence, delayed emergency laparotomy, preventable death hospital, gastrointestinal perforation claim, surgical negligence death, A&E medical negligence
Medical Negligence
Medical negligence, also known as clinical negligence (particularly in the UK), occurs when a healthcare professional provides substandard care that falls below the reasonable standard expected of a competent practitioner in similar circumstances, directly causing harm or injury to a patient.To succeed in a claim, four key elements (often referred to as the “4 Ds”) must typically be proven:
- Duty of care — A doctor-patient or similar professional relationship existed, establishing that the healthcare provider owed the patient a duty to provide competent treatment.
- Breach of duty (or deviation from the standard of care) — The care provided was negligent, meaning it did not meet the accepted professional standards. This is assessed objectively, often with input from independent medical experts, rather than requiring “gold standard” treatment.
- Causation — The breach directly caused (or significantly contributed to) the patient’s injury or worsened condition. The harm must be more likely than not attributable to the substandard care.
- Damage — The patient suffered actual harm, which may include physical injury, psychological distress, financial loss, additional medical needs, or reduced quality of life.
Common examples include misdiagnosis, delayed diagnosis, surgical errors, incorrect medication, failure to obtain informed consent, or inadequate aftercare. Not every poor outcome or medical mistake constitutes negligence—only those deviating from reasonable professional standards and causing avoidable harm qualify.In the UK, claims are pursued through the civil justice system, often against the NHS or private providers, with the goal of securing compensation to address losses and support recovery. Medical negligence cases can be complex, requiring expert evidence and strict time limits for claims.
Home Page – Medical Negligence – Medical Negligence – Medical Negligence – Home Page – Home Page – Banzai Japan – Home Page – Home Page –

https://sekaigyakuten.jp – A DePRESSeD Media Ltd Website – Cospanic Entertainment Video
- ‘Eleanor’ 64 Case Study


 English
English